Many Medicare beneficiaries are surprised when their monthly premiums suddenly increase because of income-related adjustments. If you’ve recently received a higher premium notice, understanding whether you can appeal IRMAA Medicare charges in 2026 can help you avoid paying more than necessary.
Skyline Benefit is an independent Medicare insurance broker that helps clients understand Medicare premium changes, review IRMAA notices, and explore plan strategies that may reduce overall healthcare costs.
What Is IRMAA and Why Does It Increase Medicare Premiums?
IRMAA (Income-Related Monthly Adjustment Amount) is an extra surcharge added to:
- Medicare Part B premiums
- Medicare Part D prescription drug plan premiums
This adjustment is based on your Modified Adjusted Gross Income (MAGI) from your tax return — usually from two years prior.
If your income crosses certain thresholds, Medicare considers you a higher-income beneficiary and increases your monthly costs.
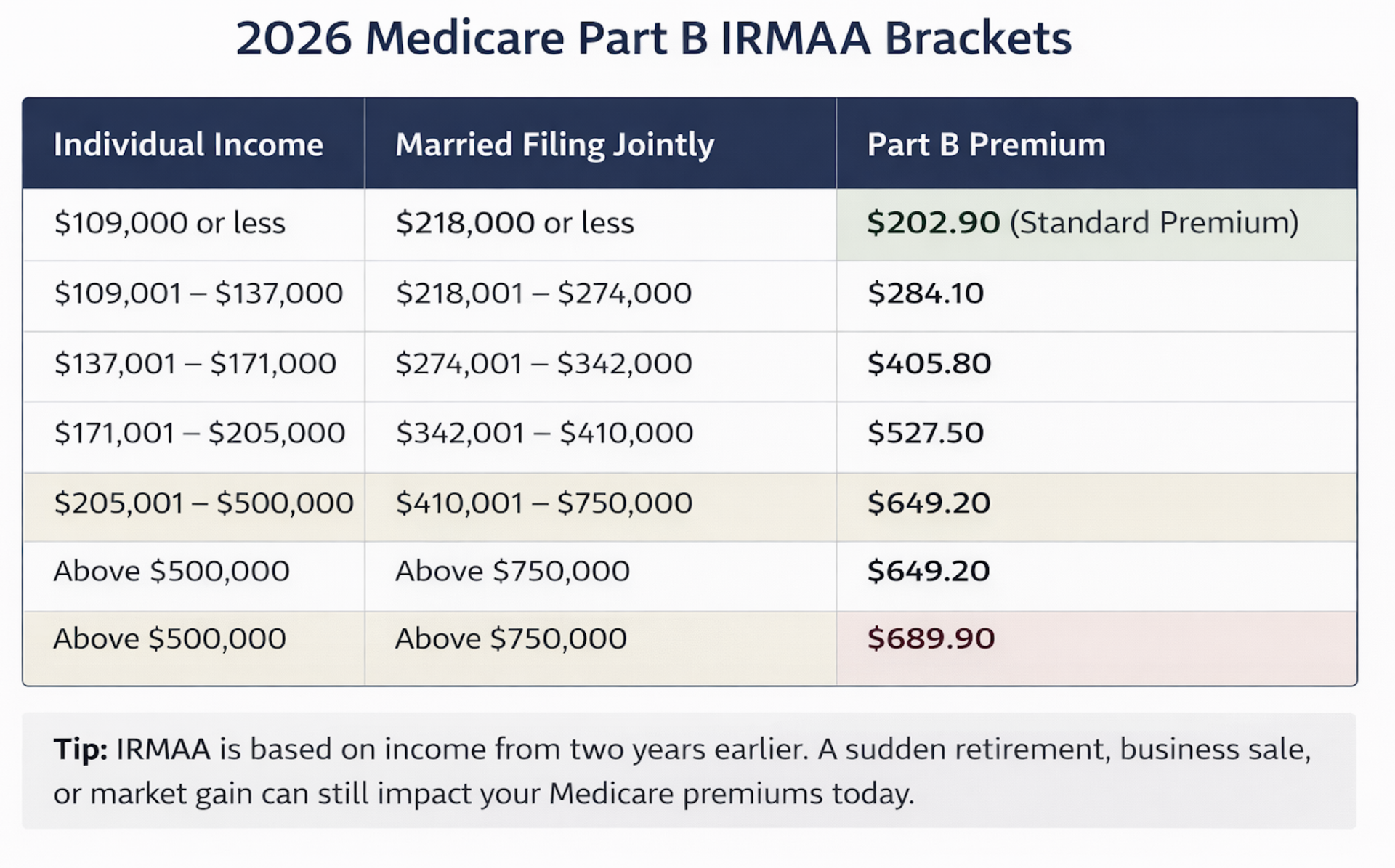
Can You Appeal IRMAA Medicare Charges in 2026?
Yes.
You can appeal IRMAA Medicare charges in 2026 if your current financial situation has changed significantly.
Social Security allows appeals when the income used to calculate your premium no longer reflects your true financial condition.
This is called filing a “Life-Changing Event” reconsideration request.
What Life Events Qualify for an IRMAA Appeal?
Medicare may reduce or remove IRMAA surcharges if you experienced certain qualifying events such as:
- Retirement or reduced work hours
- Loss of income-producing property
- Divorce or marriage
- Death of a spouse
- Pension loss
- Employer settlement payments ending
These situations can lower your current income — even if past tax returns showed higher earnings.
How Do You Appeal IRMAA Medicare Charges in 2026?
To start the appeal process, you must complete Form SSA-44.
This form allows you to:
- report your qualifying life-changing event
- estimate your current or expected income
- request a Medicare premium adjustment
You may also need to provide supporting documents such as:
- retirement letters
- employer verification
- tax projections
- financial statements
Social Security will review your case and decide whether to adjust your Medicare premium.
How Long Does an IRMAA Appeal Take?
Processing times vary, but many beneficiaries receive a decision within:
- a few weeks
- or several months depending on documentation
If approved, your Medicare premiums may be reduced retroactively, and you could receive refunds for overpaid amounts.
What If Your IRMAA Appeal Is Denied?
If your reconsideration request is denied, you still have options.
You may:
- file a formal appeal
- submit additional financial evidence
- review Medicare plan choices that better fit your budget
- evaluate drug plan costs or Medicare Advantage alternatives
Sometimes the issue is not only the IRMAA surcharge — but also overall Medicare plan structure.
Why Reviewing Your Medicare Plan Matters After an IRMAA Notice
Higher premiums can signal the need to:
- reassess prescription coverage
- compare Medicare Advantage vs Medigap options
- review provider networks
- evaluate total annual healthcare spending
Strategic Medicare planning can help offset increased premium costs.
Need Help Appealing IRMAA Medicare Charges in 2026?
Skyline Benefit helps Medicare beneficiaries understand IRMAA notices, evaluate appeal eligibility, and compare Medicare plan options that may reduce overall healthcare expenses.
If your Medicare premium recently increased, speaking with an experienced broker can help you explore practical next steps.
Call us at: (714) 888-5112

